32 Weeks Pregnant
Welcome to week 32 of your pregnancy journey! At 32 weeks pregnant, you’re a step closer to meeting your little one, and you're likely noticing some changes in both your symptoms and your bump. Your baby is maturing swiftly inside your womb, and your body is preparing itself for the beautiful yet challenging voyage of childbirth. Let's delve deeper into pregnancy at 32 weeks, exploring the common symptoms, your baby’s development, and some tips to keep both you and your baby healthy and happy.
Highlights at 32 Weeks Pregnant
Here are some of the highlights of 32 weeks pregnant:
Your baby may be about the size of a Chinese leaf cabbage at 32 weeks.
They may move into the head-down position now or in the coming weeks in preparation for birth.
It’s helpful to become familiar with the signs and symptoms of labour at 32 weeks pregnant and prepare your action plan for when the time comes.
We have some tips below on how to do those important pelvic floor exercises.
Have you found the perfect name for your baby? If not, find some inspiration by using our fun Baby Name Generator:
BABY NAME GENERATOR TOOL
Baby name generator
By gender:
By theme:
Your Baby’s Development at 32 Weeks Pregnant
Your due date is drawing near and your little one is continuing to grow and develop into the tiny human you’ll soon meet. Check out these exciting developments:
Things are starting to get a little cramped inside your bump at 32 weeks pregnant as your little one continues to plump up. The amount of amniotic fluid is also increasing, to keep your foetus at the right temperature and provide cushioning against any bumps or knocks.
The amniotic fluid has other benefits, too. Your foetus is constantly sipping from it, and then passing it out again as urine. This helps to develop the digestive system so that your baby will be able to drink breast milk or formula.
Just because space is at a premium in there, it doesn't mean that there will be any less movement. In fact, you should be feeling at least as much activity at 32 weeks pregnant as before. You should continue to feel this movement right up until you give birth. It’s important to continue tracking your baby’s movements at 32 weeks pregnant in order to familiarise yourself with their pattern and notice if their movements have slowed down or changed at all.
Your little one probably has quieter and more active periods, and even takes naps from time to time. It's important to get familiar with these patterns, and let your midwife or doctor know immediately if you notice any reduction in activity.
If closer monitoring is needed, you might be asked to count the number of kicks you feel over a set period of time. Your doctor or midwife will tell you exactly how to do this.
Meanwhile, you might like to use a kick counting chart or app if you feel it would help you get a feel for the daily patterns of activity, although this should never be used to ‘diagnose’ your foetus’s health – always consult your midwife or doctor if you have any worries.
If you’re 32 weeks pregnant with twins, check out our twin pregnancy symptoms.
What Is 32 Weeks Pregnant in Months?
How many months is 32 weeks pregnant? Well, at 32 weeks pregnant, you’re generally considered to be in your eighth month. It all depends on how you group the 40 weeks of pregnancy into 9 months, as they don’t fit neatly.
What Size Is a Baby at 32 Weeks Pregnant?
Now that you’re 32 weeks pregnant, your baby is about the size of a chinese leaf cabbage or the length of a bunch of celery. So, what does a baby measure and what is their average weight in kg at 32 weeks pregnant? At this stage, they may measure close to 42.4 centimetres from head to heel, and weigh in at around 1.7 kilograms.
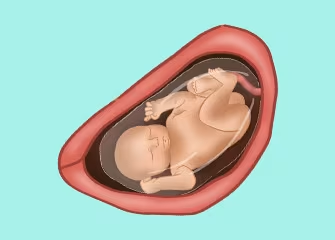
Your Baby: What Does 32 Weeks Pregnant Look Like?
The below visual is an illustration of what your little one might look like and how your baby may be positioned at 32 weeks pregnant.
Your Body at 32 Weeks Pregnant
Your bump may be pretty large and noticeable at 32 weeks pregnant, which might have an effect on those around you: People may offer their seat on public transport, and ask how many months along you are.
You may think that you're getting a little too large and uncoordinated to be doing exercise at 32 weeks, but it's important to stay as active and fit as you can.
As long as your doctor gives you the all-clear, you can actively keep fit no matter how many months pregnant you are.
If your belly is getting in the way of your usual exercise routine at 32 weeks pregnant, consider switching to a more bump-friendly way of keeping fit, such as swimming or ‘aquanatal' workouts.
If you aren't already doing them, it's never too late to start doing pelvic floor exercises. Besides strengthening a group of muscles that play a key role in labour and delivery, these exercises bring all sorts of benefits after you've had your baby.
Not only can they speed up your recovery from labour and help prevent incontinence after a vaginal birth, they may also improve sex by heightening sensitivity.
The beauty of these simple muscle clenches is that nobody can see that you're doing them – just tense up those muscles you would to stop the flow of urine, then hold for a few seconds and release.
Repeating this 10 to 15 times, 3 times a day, gradually increasing the duration of each clench, is enough to help tighten and strengthen these muscles.
If you aren't sure about how to do pelvic floor exercises, your midwife or doctor can help. They can also advise you on what other forms of exercise are still safe for you to do, or suggest ways of adapting your existing routine.
Your Symptoms at 32 Weeks Pregnant
Although every pregnancy is different, here are some of the symptoms you may experience at 32 weeks pregnant:
Swollen and sore gums. The hormones coursing through your body at the moment are making your gums more sensitive to the plaque that builds up on your teeth. If you've got swollen or bleeding gums at 32 weeks pregnant, this might be part of the cause. Because of this increased risk of gum disease, your oral hygiene is very important during pregnancy. To look after your teeth and gums, brush twice a day with fluoride toothpaste, using a soft small-headed toothbrush. Avoid sugary drinks and foods as much as you can, and ask your dentist for more advice on how to look after your teeth and gums when you're pregnant. Dental treatment provided via the NHS is free during pregnancy and for one year after your due date with a maternity exemption certificate. Your doctor or midwife can give you the form to request this.
Leg cramps. Painful spasms and cramping in your feet or calves are a common symptom that you may be experiencing at 32 weeks pregnant. They often strike at night, and nobody fully understands why. They usually go away by themselves, but you might be able to ease the pain by pulling your toes up hard towards your shins, or massaging the knotted muscle. Flexing and rotating your ankles may help prevent leg cramps, especially if you do these stretches just before bed.
Diarrhoea. It's never pleasant, but you could come down with a bout of diarrhoea at 32 weeks pregnant or at any time really. If this happens, drink plenty of water to stay hydrated. Sometimes, diarrhoea at 32 weeks pregnant can be a sign of premature labour. If you notice any symptoms like abdominal cramping, pelvic pressure, low backache, regular or painful contractions, or your water breaking at 32 weeks pregnant or beyond – with or without diarrhoea – call your midwife or doctor immediately.
What Size Is a Pregnant Belly at 32 Weeks?
You're probably getting noticeably bigger at 32 weeks pregnant, and your growing bump could be taking on a central role in your life.
As your belly grows, your centre of gravity shifts forwards, and to compensate for this you might be starting to walk with the characteristic ‘waddle' of pregnant people in the last stages of pregnancy.
What Does 32 Weeks Pregnant Look Like?
For a better idea of your belly size at 32 weeks pregnant, check out the visual below:
Things to Consider at 32 Weeks Pregnant
Here are some things for you to consider at 32 weeks pregnant:
You may be wondering how your little one is positioned. Around 32 weeks pregnant, there’s a good chance your baby is in a head-down position, but some babies also take the ‘breech’ position, which basically means they are feet or bottom-down. Don’t worry if your baby hasn’t somersaulted into a head-down position just yet. Sometimes this won’t happen until the last moment. If your baby doesn’t turn downward, your midwife or doctor might be able to help your little one move into the right position just before delivery. Even a breech presentation doesn’t always prevent a vaginal birth if that’s your preference. Lots of factors need to be considered when deciding on the safest type of delivery, including the position of the placenta and your little one’s feet. Your midwife and doctor will be monitoring your baby’s position closely, and if the shift to a head-down position hasn’t happened by around 36 weeks, they’ll discuss all the available options with you in detail.
Immediately after giving birth, you'll be offered a vitamin K injection for your baby. This is to protect against a rare bleeding disorder that can affect some newborns. Vitamin K can also be given orally, but this requires more doses. Your midwife can give you the information you need to make an informed decision. It may seem a little early to be thinking about what will happen after your baby is born, but forewarned is forearmed: At 32 weeks pregnant, now is a good time to prepare for some of the choices you'll be asked to make in the not-so-distant future.
Be on the lookout for symptoms like sudden swelling, nausea or vomiting, severe headaches, problems with vision, or pain just below the ribs at 32 weeks pregnant and throughout pregnancy. These could be signs of a rare, but potentially very serious blood pressure condition called pre-eclampsia. If you notice any of these symptoms at 32 weeks pregnant, or at any time in the rest of your pregnancy, tell your midwife or doctor straight away.
Read up on the signs of preterm labour. If you suspect you may be in preterm labour, contact your healthcare provider immediately. Your provider may be able to suggest ways that help you avoid a preterm delivery like bed rest, drinking lots of fluids, or medications that can help stop the contractions. In some cases, a hospital stay may be recommended.
Although your due date is a while off yet, it’s still a good idea to have your hospital bag packed and ready to go. Start by looking at our hospital bag checklist and then slowly start collecting everything you’ll need for a comfortable hospital stay. You might also like to ask your doctor or midwife what the hospital may provide and what they recommend you bring.
Are you familiar with the signs of labour? It's a good idea to learn what these are and to have a plan for when labour begins – your partner's doctor or midwife might discuss this with you, too. Being prepared and as informed as possible about labour, what to do next, and the delivery process may be helpful for both you and your pregnant partner.
Questions for Your Doctor at 32 Weeks Pregnant
Here are some questions you may wish to ask your doctor or midwife at 32 weeks pregnant or at any point in your third trimester:
If this isn’t my first pregnancy, will the symptoms of labour be the same as last time, and are any past pregnancy complications likely to reappear this time round?
What comfort and pain relief options are available to me during labour and delivery? What are the potential benefits and drawbacks of each option?
Is it OK to bend over at 32 weeks pregnant?
When will my baby be fully developed?
What are some symptoms not to ignore at 32 weeks pregnant?
Will I be offered an ultrasound at 32 weeks pregnant?
Can you fly at 32 weeks pregnant?
FAQS AT A GLANCE
At 32 weeks, your baby isn't fully developed yet but they're getting there! They're still gaining fat under their skin and practising breathing in preparation for the outside world. Their vital organs, like the lungs and brain, are still developing and maturing.
32 Weeks Pregnant: Your Checklist
The following checklist may come in helpful during these final weeks of pregnancy:
☐ Ask your midwife or doctor how to apply for a maternity exemption certificate if you don’t have one yet. This is valid until one year after your due date, and you’ll need it if you want to claim free NHS dental treatment and prescriptions.
☐ If a friend or loved one is hosting a baby shower for you soon and you’re planning to have a gift registry, now is a good time to prepare. Use this baby registry checklist to make sure you’ve got the essentials covered.
☐ Stock up on any baby gear and nursery essentials you’re still missing. If you haven’t already, start to plan the layout of the nursery, and think about how you'd like to decorate it.
☐ Get to know the signs and symptoms of labour at 32 weeks pregnant, so you’ll know what’s happening when the time comes.
☐ Do a practice trip to the hospital or birthing centre, so that you can time how long it takes to get there. You might want to plan some alternative routes, in case there’s a traffic jam or roadworks on the day you go into labour.
32 weeks pregnant - checklist